Clinical Operations
Our goal is to provide the best comprehensive EMS system by staying up to date on the most current practices in care for the community we service. We strive to provide the best patient care to the community by having the most state of the art equipment available. We are a growing and comprehensive EMS Department and a true 3rd service public safety organization. We are very proud of our 8,500 sq/ft station, built in 2009 that includes nearly 2,000 sq/ft dedicated to the training and education of our paramedics and staff.
The Clinical Operations Division is a multi-collaborative division compromised of the entire command staff of WCEMS. Pivotal to the success of the paramedics is the dedication and oversight assistance from Dr. William Loesch, MD. The Field Training Officers (FTO) at WCEMS are among the most important positions the department utilizes. They are the ones who carry out the education and training of the entire staff.
Clinical Capabilities
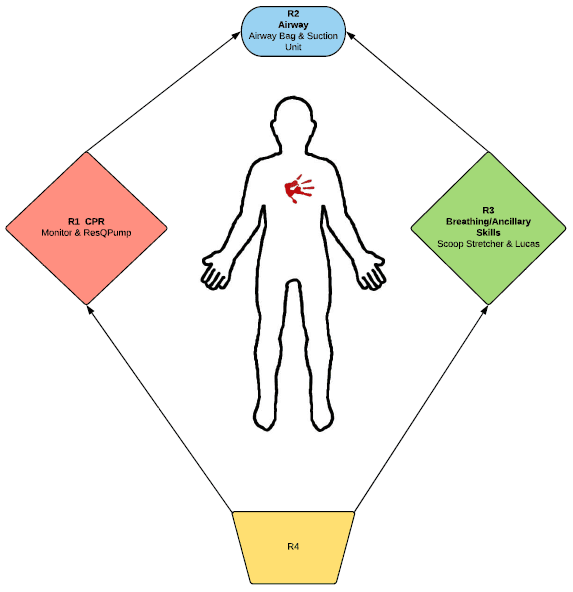 The Department of EMS realizes that without the proper medical equipment, standards of care, and right amount of clinical oversight we can not administer the best patient care to the community. The department utilizes a peer review process designed to review all aspects of the department in an organized format. Starting in 2011 we instituted the Clinical Improvement and Research Division (CIRD) comprised of field level staff and command staff designed to bring the most science proven, evidence based treatment modalities to the department. The first quarter of 2011 was focused on the evaluation and research of our current Sudden Cardiac Arrest (SCA) statistics and protocols. To see an example of how the CIRD team worked to improve CPR efficiency by implementing the pit-crew approach to rescuer positions during SCA, click the picture.
The Department of EMS realizes that without the proper medical equipment, standards of care, and right amount of clinical oversight we can not administer the best patient care to the community. The department utilizes a peer review process designed to review all aspects of the department in an organized format. Starting in 2011 we instituted the Clinical Improvement and Research Division (CIRD) comprised of field level staff and command staff designed to bring the most science proven, evidence based treatment modalities to the department. The first quarter of 2011 was focused on the evaluation and research of our current Sudden Cardiac Arrest (SCA) statistics and protocols. To see an example of how the CIRD team worked to improve CPR efficiency by implementing the pit-crew approach to rescuer positions during SCA, click the picture.
Benchmarks
In 2012, Washington County EMS implented the benchmarks. No longer are the days of “we think or believe that call went well.” We wanted a more measureable process. The benchmarks were created to measure specific critical areas for quality improvement. The areas we are monitoring at this time include; Pain Management, Cardiac Arrest, Chest Pain, RSI, Respiratory Emergencies, and Emergency Out of County Transfers.
In 2011 the department was approved a phased-in approach to bringing the new LP-15 into the hands of our paramedics. Through the financial assistance of the LCRA Community Development Partnership Grant we have also deployed the new piston driven battery powered LUCAS II mechanical CPR device. The device is just one piece in a collaborative group of improvements to the departments’ SCA protocols with the overall goal of improving ROSC (return of spontaneous circulation) and ultimately patient survival from SCA. Another improvement was the protocol addition of the MAD devices. The device gives our paramedics another route to administer life saving medications to high risk seizure patients or certain pediatric populations. In 2017 our paramedics began drawing blood cultures in the field on septic patients in order to improve patient outcome. In that year, the department obtained a Zoll EMV+ ventilator to better aid in the management of critical patients. In 2018 the department introduced the ResQPUMP to pair with the ResQPOD in order to form the ResQCPR system. We are currently working with EMSPOCUS in a study to perform ultrasound in the prehospital emergency setting. There are 5 Butterfly IQ ultrasound devices allocated to the ambulances and squads to facilitate the study. The county implemented the EleGARD into the cardiac arrest protocol as a “heads up CPR.” This will help normalize the patient’s intracranial pressure, which in turn will decrease the effects of brain injury during cardiac arrest. In 2021, whole blood made its way to Washington County EMS. This is in addition to the PRBCs that we are already carrying. This new step makes us the first EMS provider in our area to provide this valuable asset.
Whole Blood

Ultrasound

EleGARD

Advanced Community Paramedicine Program (ACP)
Washington County EMS became one of just a handful of EMS Departments in the nation to develop and utilize the Advanced Community Paramedicine (ACP) Program in Washington County. The program is an innovative way to cut healthcare costs while improving the efficiency of the healthcare system by using highly clinically skilled paramedics to fill unmet healthcare gaps in the community. The program focuses on home-visits to a growing population of patients with qualifying chronic conditions, educating these patients and their families in healthcare, and preventive practices, as well as navigating patients to the most appropriate care facilities and resources for their individual needs. The program has already saved over $1,600,000 from our 2013 budget proposal and we expect that to increase as the program continues.
To read more about the program click here..
